
27 June 2023
Attention-Deficit/Hyperactivity
Disorder (ADHD)
Attention-Deficit/Hyperactivity Disorder (ADHD) is a neurodevelopmental disorder that
affects both children and adults. It is characterized by persistent patterns of inattention,
hyperactivity, and impulsivity that can significantly impact various aspects of an individual's
life, including academic performance, work productivity, and social relationships. In this article,
we will explore ADHD in depth, including its definition, prevalence, causes, symptoms, diagnosis,
and treatment options.
Introduction to ADHD
Definition of Attention-Deficit/Hyperactivity Disorder ADHD
DHD, which stands for Attention-Deficit/Hyperactivity Disorder, is a neurodevelopmental
disorder characterized by persistent patterns of inattention, hyperactivity, and impulsivity
that are significantly impairing and inconsistent with the individual's developmental level.
It is typically diagnosed in childhood but can persist into adulthood.
Historical background
The historical understanding of ADHD has evolved over time, with
changes in terminology, diagnostic criteria, and societal perceptions. Here is a brief
overview of the historical background of ADHD:
Early Observations (Late 18th to Early 20th Century):
In the late 18th century, physician Sir Alexander Crichton described a condition
called "mental
restlessness" characterized by symptoms similar to ADHD.
In the early 20th century, Sir George F. Still, a British pediatrician, provided detailed
clinical descriptions of children who exhibited inattentiveness, impulsivity, and hyperactivity.
Minimal Brain Dysfunction (1960s):
In the 1960s, research focused on the relationship between brain dysfunction
and behavioral
difficulties, leading to the concept of Minimal Brain Dysfunction (MBD).
MBD encompassed a range of cognitive and behavioral issues, including what is now recognized
as
ADHD.
Hyperkinetic Reaction of Childhood (1970s):
In the 1970s, the term "Hyperkinetic Reaction of Childhood" was introduced as a
diagnostic
label.
The emphasis was on hyperactivity and motor restlessness, and the condition was believed to
be
caused by environmental factors.
Attention Deficit Disorder (ADD) and Attention-Deficit/Hyperactivity Disorder (ADHD)
(1980s):
In 1980,
the Diagnostic and Statistical Manual of Mental Disorders,
Third Edition (DSM-III)
introduced the term "Attention Deficit Disorder" (ADD) to describe the
predominantly inattentive
presentation.
In 1987, the DSM-III-R
expanded the diagnostic criteria and introduced the term
"Attention-Deficit/Hyperactivity Disorder" (ADHD), encompassing both inattention and
hyperactivity/impulsivity.
DSM-IV and DSM-5 (1990s and 2010s):
The Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition
(DSM-IV, 1994) refined
the diagnostic criteria and introduced subtypes of ADHD.
In 2013, the DSM-5 was published, merging the subtypes into three presentations:
predominantly
inattentive, predominantly hyperactive-impulsive, and combined presentation.
Prevalence and
demographics
ADHD is a common neurodevelopmental disorder that affects both children and
adults worldwide. Here is an overview of the prevalence and demographics of ADHD:
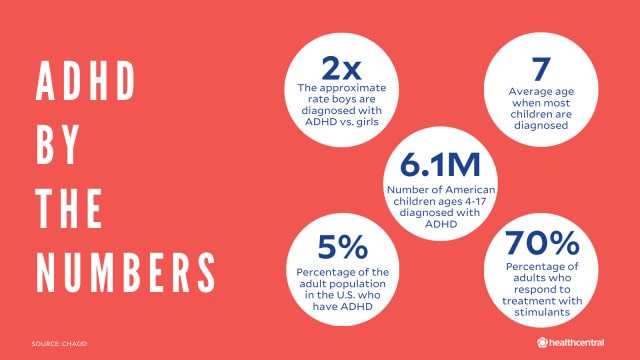
Prevalence:
The estimated global prevalence of ADHD in children is around 5-7%. However, prevalence rates
can vary across countries and regions.
In adults, the estimated prevalence of ADHD is lower, ranging from 2-5%.
It's important to note that ADHD can persist into adulthood, and many individuals may go
undiagnosed or misdiagnosed.
Gender Differences:
In childhood, ADHD is more commonly diagnosed in boys than girls. Boys are typically diagnosed
at a ratio of 2-3:1 compared to girls.
However, research suggests that the ratio may be closer to 1:1 in adults, indicating that ADHD
might be underdiagnosed or overlooked in females.
Age of Onset:
ADHD symptoms typically appear in early childhood, with the average age of onset around 7 years
old.
Some individuals may exhibit symptoms as early as preschool age, while others may not receive a
diagnosis until adolescence or adulthood.
Developmental Course:
ADHD symptoms can change over time as individuals mature and develop coping mechanisms.
In some cases, symptoms may improve or diminish, while others may experience ongoing challenges
throughout their lives.
The presentation of symptoms may also change, with hyperactivity and impulsivity symptoms often
decreasing with age, while inattention symptoms may persist.
Comorbidity:
ADHD commonly coexists with other mental health disorders. The most common comorbidities include
oppositional defiant disorder (ODD), conduct disorder (CD), anxiety disorders, mood disorders,
and learning disabilities.
Comorbid conditions can complicate diagnosis, treatment, and overall functioning.
Cultural and Geographical Variations:
The prevalence and diagnosis rates of ADHD can vary across different cultural
and geographical contexts.
Factors such as cultural norms, diagnostic practices, access to healthcare, and awareness of
ADHD may influence prevalence rates and diagnostic patterns.
Understanding the prevalence and demographics of ADHD helps shed light on the
impact of the disorder and the need for appropriate diagnosis, treatment, and support for
affected individuals. It also emphasizes the importance of raising awareness and reducing
stigma surrounding ADHD.
Impact of ADHD on
individuals and society
ADHD (Attention-Deficit/Hyperactivity Disorder) has a significant impact on
individuals and
society. For individuals, ADHD can lead to academic difficulties, impaired occupational
functioning, challenges in social relationships, and emotional struggles. Academic
performance
may suffer due to inattention and poor organization, leading to lower grades and academic
underachievement. In the workplace, ADHD can affect productivity, job performance, and
career
stability. Socially, individuals with ADHD may experience difficulties in making and
maintaining
relationships, leading to social isolation and rejection. The emotional well-being of
individuals with ADHD can be compromised due to repeated challenges and potential comorbid
mental health disorders.
On a societal level, ADHD imposes economic burdens through healthcare costs, educational
support
needs, and social services. The costs associated with diagnosis, treatment, and
interventions
can be substantial. Additionally, ADHD affects educational and employment systems, requiring
resources and support services. The stigma surrounding ADHD can contribute to
misunderstandings
and barriers to accessing appropriate support.
Addressing the impact of ADHD requires early identification, accurate diagnosis, and
comprehensive management approaches. Providing effective interventions, raising awareness,
and
reducing stigma can help individuals with ADHD reach their full potential and enhance their
overall well-being. It also necessitates investment in healthcare, education, and social
support
systems to cater to the needs of individuals with ADHD and mitigate the societal impact of
the
disorder.
Symptoms and Subtypes
of ADHD
Inattention symptoms
Difficulty sustaining attention and easily getting distracted.
Trouble organizing tasks and activities.
Forgetfulness and frequently losing things.
Avoidance or reluctance to engage in tasks that require sustained mental effort.
Hyperactivity symptoms
Restlessness, fidgeting, or excessive movement.
Difficulty staying seated and feeling a constant need to move.
Excessive talking and difficulty waiting for turns.
Often "on the go" or appearing driven by a motor.
Impulsivity symptoms
6 Acting without thinking and engaging in risky behaviors.
Difficulty with impulse control and interrupting others.
Blurting out answers or comments before the question is complete.
Difficulty adhering to rules or instructions.
Based on the
predominant symptomatology, ADHD is categorized into three subtypes:
Predominantly inattentive presentation
Individuals primarily exhibit symptoms of inattention without significant
hyperactivity or
impulsivity.
They may have trouble staying focused, organizing tasks, and following through on
instructions.
This subtype is more common in girls and may go unnoticed or be misdiagnosed due to the
absence of hyperactive behaviors.
Predominantly hyperactive-impulsive presentation
Individuals primarily exhibit symptoms of hyperactivity and impulsivity without
significant
inattention.
They may be restless, talkative, and have difficulty controlling their impulses.
This subtype is more common in boys and is often recognized earlier due to the noticeable
hyperactive behaviors.

27 June 2023
Risk Factors
Researchers are not sure what causes ADHD, although many studies suggest that genes
play a large role. Like many other disorders, ADHD probably results from a combination of
factors. In addition to genetics, researchers are looking at possible environmental factors that
might raise the risk of developing ADHD and are studying how brain injuries, nutrition, and
social environments might play a role in ADHD.
ADHD is more common in males than females, and females with ADHD are more likely to primarily
have inattention symptoms. People with ADHD often have other conditions, such as learning
disabilities, anxiety disorder, conduct disorder, depression, and substance use disorder.
While there is no cure for ADHD, currently available treatments may reduce symptoms
and improve functioning. Treatments include medication, psychotherapy, education or training, or
a combination of treatments.
Medication
For many people, ADHD medications reduce hyperactivity and impulsivity and improve their ability
to focus, work, and learn. Sometimes several different medications or dosages must be tried
before finding the right one that works for a particular person. Anyone taking medications must
be monitored closely by their prescribing doctor.
Stimulants. The most common type of medication used for treating
ADHD is called a “stimulant.”
Although it may seem unusual to treat ADHD with a medication that is considered a stimulant,
it
works by increasing the brain chemicals dopamine and norepinephrine, which play essential
roles
in thinking and attention.
Under medical supervision, stimulant medications are considered safe. However, like all
medications, they can have side effects, especially when misused or taken in excess of the
prescribed dose, and require an individual’s health care provider to monitor how they may be
reacting to the medication.
Non-stimulants. A few other ADHD medications are non-stimulants.
These medications take longer
to start working than stimulants, but can also improve focus, attention, and impulsivity in
a
person with ADHD. Doctors may prescribe a non-stimulant: when a person has bothersome side
effects from stimulants, when a stimulant was not effective, or in combination with a
stimulant
to increase effectiveness.
Although not approved by the U.S. Food and Drug Administration (FDA) specifically for the
treatment of ADHD, some antidepressants are used alone or in combination with a stimulant to
treat ADHD. Antidepressants may help all of the symptoms of ADHD and can be prescribed if a
patient has bothersome side effects from stimulants. Antidepressants can be helpful in
combination with stimulants if a patient also has another condition, such as an anxiety
disorder, depression, or another mood disorder. Non-stimulant ADHD medications and
antidepressants may also have side effects.
Doctors and patients can work together to find the best medication, dose, or medication
combination. Learn the basics about stimulants and other mental health medications on the
NIMH
Mental Health Medications webpage and check the FDA website for the latest medication
approvals,
warnings, and patient information guides.
Psychotherapy and Psychosocial Interventions
Several specific psychosocial interventions have been shown to help individuals with ADHD and their
families manage symptoms and improve everyday functioning.
For school-age children, frustration, blame, and anger may have built up within a family before a
child is diagnosed. Parents and children may need specialized help to overcome negative feelings.
Mental health professionals can educate parents about ADHD and how it affects a family. They also
will help the child and his or her parents develop new skills, attitudes, and ways of relating to
each other.
All types of therapy for children and teens with ADHD require parents to play an active role.
Psychotherapy that includes only individual treatment sessions with the child (without parent
involvement) is not effective for managing ADHD symptoms and behavior. This type of treatment is
more likely to be effective for treating symptoms of anxiety or depression that may occur along with
ADHD.
Behavioral therapy is a type of psychotherapy that aims to help a person change their behavior. It
might involve practical assistance, such as help organizing tasks or completing schoolwork, or
working through emotionally difficult events.
Behavioral therapy also teaches a person how to:
Monitor their own behavior
Give oneself praise or rewards for acting in a desired way, such as controlling anger or thinking
before acting
Parents, teachers, and family members also can give feedback on certain behaviors and help establish
clear rules, chore lists, and structured routines to help a person control their behavior.
Therapists may also teach children social skills, such as how to wait their turn, share toys, ask
for help, or respond to teasing. Learning to read facial expressions and the tone of voice in
others, and how to respond appropriately can also be part of social skills training.
Cognitive behavioral therapy helps a person learn how to be aware and accepting of one’s own
thoughts and feelings to improve focus and concentration. The therapist also encourages the person
with ADHD to adjust to the life changes that come with treatment, such as thinking before acting, or
resisting the urge to take unnecessary risks.
Family and marital therapy can help family members and spouses find productive ways to handle
disruptive behaviors, encourage behavior changes, and improve interactions with the person with
ADHD.
Parenting skills training (behavioral parent management training) teaches parents skills for
encouraging and rewarding positive behaviors in their children. Parents are taught to use a system
of rewards and consequences to change a child’s behavior, to give immediate and positive feedback
for behaviors they want to encourage, and to ignore or redirect behaviors they want to discourage.
Specific behavioral classroom management interventions and/or academic accommodations for children
and teens have been shown to be effective for managing symptoms and improving functioning at school
and with peers. Interventions may include behavior management plans or teaching organizational or
study skills. Accommodations may include preferential seating in the classroom, reduced classwork
load, or extended time on tests and exams. The school may provide accommodations through what is
called a 504 Plan or, for children who qualify for special education services, an Individualized
Education Plan (IEP).
Stress management techniques can benefit parents of children with ADHD by increasing their ability
to deal with frustration so that they can respond calmly to their child’s behavior.



